Congenital epidermolysis bullosa
Congenital epidermolysis bullosa (EB) —also called the “butterfly skin disease”— is a group of rare diseases with skin fragility characterized by structural anomalies that reduce the resilience of skin, causing painful, open wounds that appear either spontaneously or due to friction.
Blisters and erosions/ulcers may appear in these patients in response to a minor injury, even from heat, rubbing, scratching, or adhesive tape. In severe cases, blisters and erosions/ulcers may occur inside the body, such as the lining of the mouth or the stomach.
The four major kinds of congenital epidermolysis bullosa are congenital EB simplex -the most common kind, developed in the outer layer of skin; congenital junctional EB, a potentially severe disorder characterized by blisters between the dermis and the epidermis, affecting the skin and mucosa;congenital dystrophic EB, related to a flaw in the gene collagen VII, which helps produce a protein that glues dermis and epidermis together; and Kindler syndrome.
It tends to cause blisters in different skin layers, so it can look very different from person to person. The condition usually shows up in infancy or early childhood. Some people do not develop signs and symptoms until adolescence or early adulthood. Currently, the overall prevalence of the different kinds of congenital epidermolysis bullosa is approximately 11 affected subjects per one million people.



Congenital epidermolysis bullosa
Epidermolysis bullosa is classified into four primary types based on the depth of the skin layer where blistering occurs: EB Simplex, the most common and generally least severe form, where the split occurs in the outermost layer (epidermis); Junctional EB, a severe variant where blistering happens within the basement membrane zone; Dystrophic EB, which occurs in the deeper dermis and leads to permanent scarring and physical deformities; and Kindler Syndrome, a rare type where blistering can happen across multiple layers and is accompanied by light sensitivity. Essentially, the deeper the structural defect, the more significant the complications.
What causes congenital epidermolysis bullosa?
Congenital epidermolysis bullosa has a genetic origin. The disease gene may be passed on from one parent who has the disease (autosomal dominant inheritance), or it may be passed on from both parents that are carriers (autosomal recessive inheritance) or arise as a new mutation in the affected person that can be passed on. For example, dystrophic congenital EB may be inherited as a dominant or recessive trait; generally, the recessive form, RDEB, is more severe than the dominant disease, DDEB.
The skin is made up of an outer layer (epidermis) and an underlying layer (dermis). The area where the layers meet is called the basement membrane. The various types of congenital epidermolysis bullosa are largely defined by which layer the blisters form in.

How is epidermolysis bullosa diagnosed?
The diagnosis of congenital epidermolysis bullosa begins with a clinical suspicion, typically triggered when a healthcare professional observes unexplained blistering or skin fragility in a newborn or young child. Because the condition can resemble other skin disorders, doctors must look for specific patterns of blisters that form specifically in response to friction or minor trauma. To confirm the diagnosis and determine the specific subtype, laboratory tests are essential.
How is congenital epidermolysis bullosa detected?
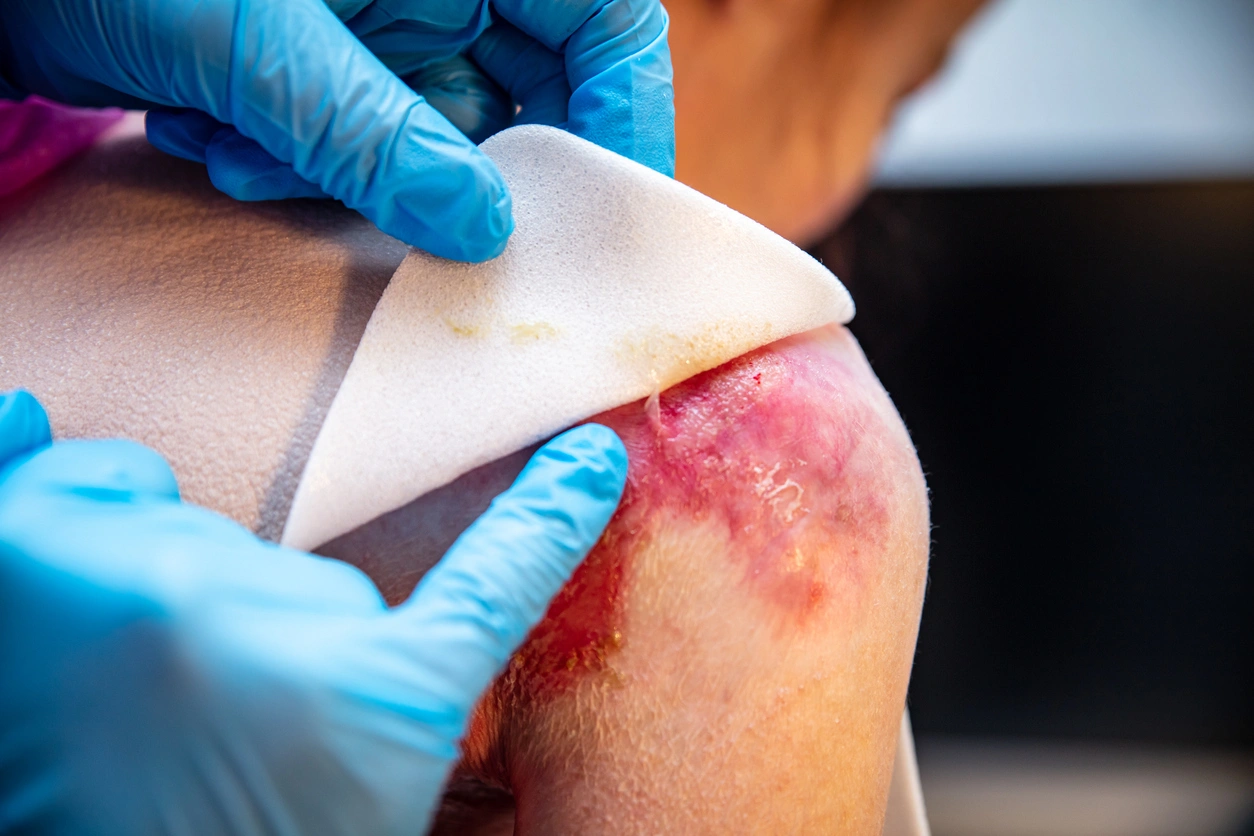
Patients with congenital epidermolysis bullosa have fragile skin that blisters very easily. At the slightest trauma, lesions occur in the form of blisters and/or erosions/ulcerations that can sometimes form scars when they heal. When present, these can be prominent and complex and may entail retraction of the surrounding skin. Blisters or lesions may appear all over the body, on the outer layer of the skin, but also in the mucosa, such as the mouth, the nose, the eyes, etc.
References
- Debra Org. EB in Depth. 2020 January [Revised 2020 March]. Available at: https://www.debra.org/about-eb/eb-depth
- Mayo Clinic. Epidermolysis Bullosa. 2018 March [Revised 2020 March]. Available at: https://www.mayoclinic.org/diseases-conditions/epidermolysis-bullosa/symptoms-causes/syc-20361062
- Medline Plus. Epidermolysis Bullosa. 2018 October [Revised 2020 March]. Available at: https://medlineplus.gov/ency/article/001457.htm
- Fine JD. Epidemiology of Inherited Epidermolysis Bullosa Based on Incidence and Prevalence Estimates From the National Epidermolysis Bullosa Registry. JAMA Dermatol. 2016 Nov 1;152(11):1231-1238. doi: 10.1001/jamadermatol.2016.2473. PMID: 27463098.
- Has C. et al. Consensus reclassification of inherited epidermolysis bullosa and other disorders with skin fragility. Br J Dermatol. 2020 Oct;183(4):614-627. doi: 10.1111/bjd.18921. Epub 2020 Mar 11. PMID: 32017015.