Congenital epidermolysis bullosa treatments

What are the main treatments for congenital epidermolysis bullosa?
Care for EB relies on a comprehensive and coordinated approach. Most patients benefit from care provided by a multidisciplinary team that may include dermatologists, specialist nurses, dietitians, pain specialists, physiotherapists, and occupational therapists. These professionals address both daily symptoms and long-term complications.
Wound care forms the cornerstone of EB management. Gentle handling of the skin and consistent routines help reduce pain, prevent infection, and support healing.
Blister care
Clinicians often advise draining new blisters with sterile equipment to stop them spreading. Keeping the blister roof intact protects the underlying skin and acts as a natural barrier.
Appropriate dressings
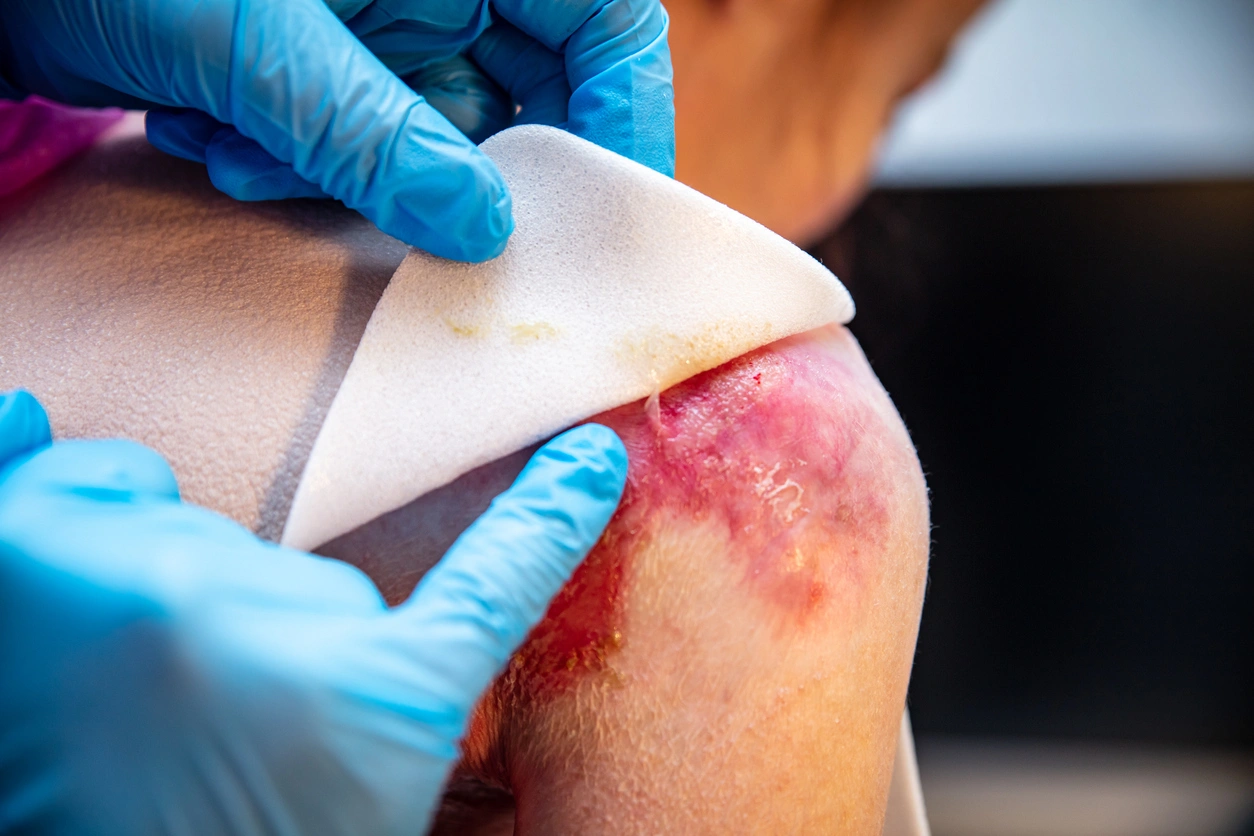
Non-adhesive, soft dressings protect fragile skin and minimize trauma during removal. These dressings reduce friction, absorb wound fluid, and promote healing.
Daily skin care
Regular use of moisturizers and emollients keeps the skin supple and reduces cracking. Loose, soft clothing and careful positioning also lower the risk of new injuries.
Starting good wound care early in life can reduce discomfort and limit long-term scarring.
Infection prevention and management
Open wounds create an ongoing risk of infection, which can delay healing and worsen pain. To reduce this risk, clinicians use antiseptic solutions to control bacteria on the skin and prescribe topical antibiotics when local infection develops. If signs suggest a deeper or spreading infection, doctors may recommend oral or intravenous antibiotics. Regular dressing changes and careful inspection of wounds help identify early warning signs such as redness, swelling, or discharge. Prompt treatment of infection plays a key role in preventing serious complications.
Pain control and symptom relief
Pain represents one of the most challenging aspects of EB and often requires an individualized plan. Mild pain may respond to medicines such as paracetamol, while more severe pain often requires prescription analgesics. Dressing changes and wound care can also cause significant discomfort. Healthcare teams use local or systemic pain relief to make these procedures more manageable. Effective pain control improves sleep, mobility, and overall wellbeing.
Nutritional support and adjuvant therapies
EB can interfere with eating and digestion, particularly when blisters affect the mouth or oesophagus. But good nutrition supports wound healing and growth, especially in children. This is why dietitians help ensure adequate intake of calories, protein and essential nutrients, and feeding strategies may be needed for some infants and children who require modified feeding techniques or nutritional supplements to meet their needs.
Physiotherapists and occupational therapists also play an important role. They advise on safe movement, prevent joint stiffness and recommend adaptations that protect the skin during daily activities.
Surgical interventions
Surgery does not treat EB itself, but it can relieve complications that develop over time. For example, scarring may cause fingers or toes to fuse together, and surgical separation can restore movement and function. EB can also lead to scarring inside the oesophagus, which narrows the passage and makes swallowing difficult; balloon dilation can widen the oesophagus and support better swallowing and nutritional intake. These procedures address specific functional problems and often improve quality of life.
Topical and gene-based therapies
Recent advances have expanded treatment options beyond supportive care.
- Topical gene therapy: certain gels can be used to deliver corrective genetic material directly to chronic wounds. In selected EB types, these treatments can speed up healing and reduce blister duration.
- Cell-based gene therapy: this approach involves correcting a patient’s own skin cells in the laboratory and grafting them back onto affected areas. Approved therapies of this kind mark a major step towards treating the underlying cause of EB, rather than only its symptoms.
- Experimental treatments: clinical trials continue to explore stem-cell therapies, protein replacement and repurposed medicines that may further improve healing or slow disease progression.
These innovations signal a shift towards biologically targeted care in congenital epidermolysis bullosa.
References
- National Health Service (NHS). Epidermolysis bullosa: Treatment. NHS [Internet]. 2021 Jun 23 [cited 2025 Dec 15]. Available from: https://www.nhs.uk/conditions/epidermolysis-bullosa/treatment/
- Siañez-González C, Pezoa-Jares R, Salas-Alanis JC. Congenital epidermolysis bullosa: A review. Actas Dermosifiliogr. 2009 Dec;100(10):842-856 [cited 2025 Dec 15]. Available from: https://www.actasdermo.org/es-congenital-epidermolysis-bullosa-a-review-articulo-S1578219009705542
- American Academy of Dermatology Association. Epidermolysis bullosa: Diagnosis and treatment. AAD [Internet]. 2024 Jun 7 [cited 2025 Dec 15]. Available from: https://www.aad.org/public/diseases/a-z/epidermolysis-bullosa-treatment