Congenital Epidermolysis bullosa triggering factors

Congenital epidermolysis bullosa triggering factors
Patients with congenital epidermolysis bullosa (EB) suffer from extremely delicate skin that can develop painful blisters and open wounds. The condition primarily affects the skin, but it can also involve internal linings such as the mouth, throat, and oesophagus. The triggering factors of congenital epidermolysis bullosa are a combination of genetic vulnerability and external physical stress. While genes determine whether EB develops, everyday mechanical forces determine when and where blisters appear. Understanding this distinction helps patients, families and healthcare professionals reduce injury and manage the signs and symptoms of congenital epidermolysis bullosa more effectively.
What is the cause of congenital epidermolysis bullosa?
Epidermolysis bullosa develops because of inherited mutations in genes responsible for proteins that give skin its strength and resilience. These proteins form a structural network that binds the outer layer of the skin, known as the epidermis, to the deeper dermis. When these proteins do not work properly or are missing altogether, the layers of the skin lose their normal stability. As a result, the skin tears and blisters under stresses that healthy skin would tolerate without difficulty.
There are four different types of epidermolysis bullosa depending on the depth at which the skin separates, and the specific gene involved: epidermolysis bullosa simplex (EBS), junctional EB (JEB), dystrophic EB (DEB), and Kindler syndrome.
Some forms of EB occur when a child inherits a single altered gene from one parent, known as autosomal dominant inheritance. Other forms require two altered copies of a gene, one from each parent, which is described as autosomal recessive inheritance. In a small number of cases, EB results from a new genetic mutation that arises spontaneously, even when neither parent shows signs of the condition.
Researchers have linked inherited EB to mutations in more than a dozen genes, and ongoing genetic studies continue to identify additional variants that contribute to the condition.
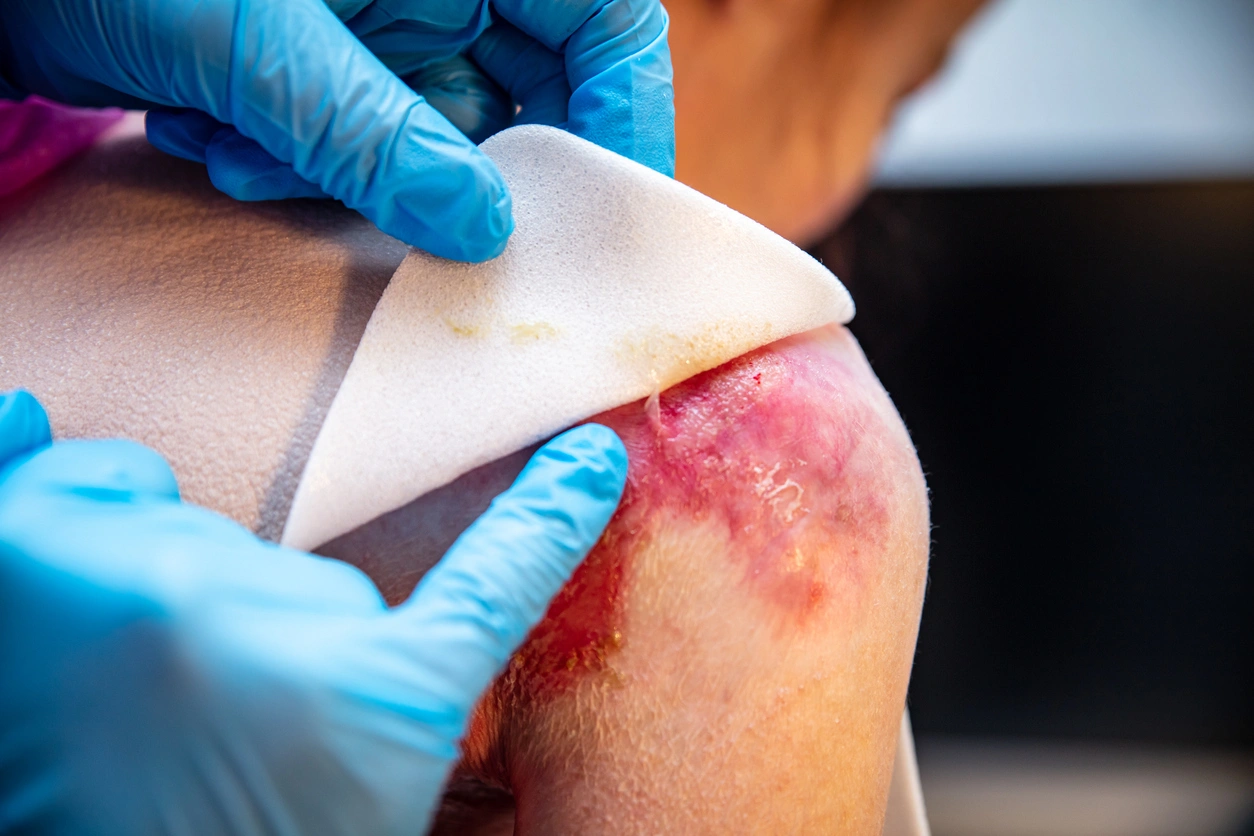
What triggers epidermolysis bullosa?
Although genetics determine whether someone has congenital EB, the actual blistering episodes occur in response to external triggers, even if these are minimal. These triggers are primarily mechanical forces acting on skin that lacks normal structural support. Because the proteins that normally absorb and distribute stress are defective, even mild friction or pressure can cause the skin layers to separate and form blisters.
Mechanical friction and trauma
Everyday physical contact represents the most common trigger for blister formation in EB. Normal movements such as crawling, walking, gripping objects, or changing position can create enough shear force to damage such fragile skin. Contact with clothing seams, footwear, or bedding can also provoke blistering and wounds. These triggers often appear early in life, sometimes from birth, as soon as the child begins to move and interact with their surroundings.
Blisters tend to develop in areas exposed to repeated friction or pressure. Common sites include the hands, feet, elbows, knees, neck, and nappy area in infants. In these regions, skin layers separate easily because they lack the resistance found in unaffected skin.
Heat, sweating and adhesive materials
Heat and moisture further increase the risk of blistering. Warm environments promote sweating, which softens the outer skin layer and increases friction between skin surfaces. Heat can also exaggerate movement between the epidermis and dermis, making blister formation more likely.
Certain materials act as additional triggers. Adhesive tapes, rough fabrics, and poorly fitted clothing can stick to or rub against fragile skin, leading to tearing and blistering. For this reason, careful selection of soft clothing, non-adhesive dressings, and gentle bandaging techniques play a central role in managing EB on a daily basis.
Internal movements and mucosal stress
EB does not affect only the outer skin. In many patients, it also involves mucosal surfaces inside the body. Normal actions such as eating, swallowing, and speaking can place stress on the delicate lining of the mouth, throat and oesophagus. This can result in internal blistering, pain, and difficulty swallowing, which may contribute to poor nutrition and delayed growth, particularly in children.
Secondary triggering factors
Some factors do not directly cause new blisters but increase the likelihood of skin damage when combined with mild mechanical stress. Dehydration and dry skin reduce elasticity, making the skin less able to tolerate movement. Inflammation around existing wounds can also weaken surrounding tissue and lower the threshold for further blistering. While these influences do not cause EB, they can worsen symptoms and increase blister frequency when the condition is already present.
It is important to clarify what does not trigger congenital EB. The condition does not result from infections, contagious exposure, or lifestyle choices. External factors alone cannot cause EB in someone who does not carry the relevant genetic mutation. Genetics create the lifelong susceptibility, while physical stress determines how the disease manifests day to day.
References
- Medicover Genetics. Butterfly skin explained: understanding epidermolysis bullosa [Internet]. Available from: https://medicover-genetics.com/butterfly-skin-explained-understanding-epidermolysis-bullosa/
- Fine JD, Mellerio JE. Congenital epidermolysis bullosa: a review. Actas Dermo-Sifiliográficas [Internet]. Available from: https://www.sciencedirect.com/science/article/pii/S0022202X21022739
- American Academy of Dermatology Association. Epidermolysis bullosa causes [Internet]. Available from: https://www.aad.org/public/diseases/a-z/epidermolysis-bullosa-causes