Psoriasis
Psoriasis is a chronic, non-contagious inflammatory disease that primarily affects the skin and nails and is associated with other health conditions known as comorbidities. On the skin, psoriasis appears as localized or generalized patches (plaques). These plaques are typically flaky, itchy, and scaly and can be red or pink on lighter skin and purple, brown or gray on darker skin tones. Plaques commonly affect the elbows, knees, scalp, and lower back, but can appear anywhere.
In addition, people with psoriasis are more likely to have other chronic conditions known as comorbidities, such as cardiometabolic disease (e.g., heart disease, high blood pressure, diabetes), inflammatory bowel disease, kidney disease, and anxiety or depression.
Psoriasis can cause a physical, emotional and social burden, affecting daily life. Additionally, social exclusion, discrimination and stigma can also have a high impact on the person living with psoriasis and their family.

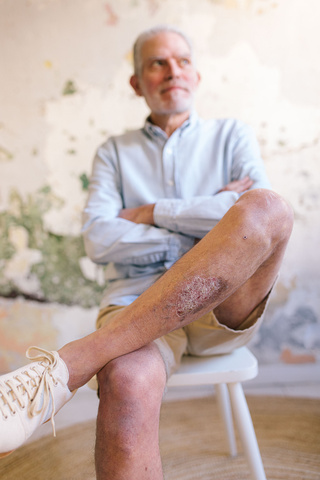

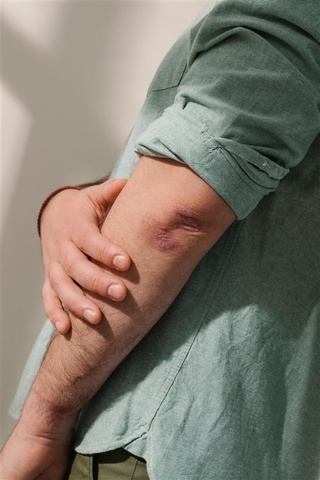
Types of psoriasis
The most common type is plaque psoriasis. Other types of psoriasis include guttate (small, drop-shaped spots), inverse (skin folds), pustular (pustules on red skin), and erythrodermic (rare, severe, needs urgent care).
Psoriasis is a lifelong condition. Periods when the plaques appear or worsen are called flare-ups and periods when they disappear are called remissions. Remission does not necessarily mean that the disease is cured, this resolution is only temporary and flare-ups can return. It can also affect the nails and, in some people, the joints and tendon insertions, causing psoriatic arthritis, with joint pain, swelling and stiffness.

Ilse, living with Psoriasis
Why does psoriasis occur?
The exact cause of psoriasis is not fully understood, but several factors are believed to contribute to its development, including:
- Genetics: certain inherited genetic changes can increase the likelihood of developing psoriasis.
- Immune system: in psoriasis, the immune system becomes overactive and immune signals in the skin become unbalanced accelerating the skin cell turnover cycle.
- Triggering factors: psoriasis can be triggered by both internal and external factors, such as minor skin injuries, sunburn, infections, certain medications, lifestyle habits and periods of psychological stress.
Psoriasis cannot be prevented. However, understanding and minimizing these triggers can reduce the likelihood or intensity of flare-ups.

Ivet, living with Psoriasis
How is psoriasis diagnosed?
Psoriasis is usually diagnosed by examining the skin. However, when the lesions are atypical or in case of doubt, a small skin biopsy may be taken and analyzed to confirm the diagnosis.
To decide on treatments, doctors look at how much skin is affected and how severe the patches are. They also check if psoriasis is in high-impact areas such as the face, hands, feet, genitals, nails, or scalp. Other important factors include how much it affects daily life and whether there are joint symptoms.
Signs and symptoms of psoriasis
Psoriasis manifests primarily as raised, red patches of skin covered with silvery-white scales, known as plaques. You will typically find these on the elbows, knees, scalp, and lower back, though they can appear anywhere on the body. These patches often feel itchy or sore, and in severe cases, the skin may crack and bleed. You might also notice changes to your nails, such as small dents called "pitting," discoloration, or the nail lifting away from the bed. Many people also experience stiff, swollen, or painful joints, a condition known as psoriatic arthritis, which often accompanies the skin symptoms.
References
- Feldman, S.R. Psoriasis: Epidemiology, clinical manifestations, and diagnosis. UpToDate [Internet]. 2020 [Cited 2020 Jan 31]. Available at: https://www.uptodate.com/contents/psoriasis-epidemiology-clinical-manifestations-and-diagnosis
- Feldman, S.R. Treatment of psoriasis in adults. UpToDate [Internet]. 2020 [Cited 2020 Feb 13]. Available at: https://www.uptodate.com/contents/treatment-of-psoriasis-in-adults
- Kang, S., Amagai, M., Bruckner, A.L., Enk, A.H., Margolis, D.J., McMichael, A.J., Orringer, J.S. Fitzpatrick’s Dermatology. McGraw Hill. 9th. ed. Buenos Aires, Argentina: Editorial Médica Panamericana S.A.; 2009. 720 p.
- World Health Organization (WHO). Global report on psoriasis [Internet]. 2016. Available at: https://apps.who.int/iris/handle/10665/204417
- Global Psoriasis Atlas (GPA). Key messages [Internet]. 2020. Available at: https://globalpsoriasisatlas.org/key-messages
- National Psoriasis Foundation (NPF). About psoriasis [Internet]. 2020 Mar 8. Available at: https://www.psoriasis.org/about-psoriasis
- National Psoriasis Foundation (NPF). Gluten-Free Diet [Internet]. 2019. Available at: https://www.psoriasis.org/treating-psoriasis/complementary-and-alternative/diet-and-nutrition/gluten-free-diet
- Barrea, L., Nappi, F., Di Somma, C., Savanelli, M.C., Falco, A., Balato, A., et al. Environmental Risk Factors in Psoriasis: The Point of View of the Nutritionist. Int J Environ Res Public Health [Internet]. 2016 Jul;13(7):743. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4962284/. doi: 10.3390/ijerph13070743
- European Academy of Dermatology and Venereology (EADV). Psoriasis can be hereditary [Internet]. 2019. Available at: https://www.eadv.org/cms-admin/showfile/9635-EADV%20PSORIASIS-7-Psoriasis%20and%20genetics.pdf
- Gudjonsson, J.E., Elder, J.T. Chapter 28: Psoriasis [Internet]. 2019. Available at: https://accessmedicine.mhmedical.com/content.aspx?sectionid=210417798&bookid=2570&R esultclick=2
- Psoriasis Health Indicator Report 2024. National Psoriasis Foundation. USA. Available at: https://www.psoriasis.org/health -indicator -report
- Parisi R, et al. Global Psoriasis Atlas. National, regional, and worldwide epidemiology of psoriasis: systematic analysis and modelling study. BMJ. 2020; 369:m1590
- Psoriasis Health Indicator Report 2024. National Psoriasis Foundation. USA. Available at: https://www.psoriasis.org/health -indicator -report
- Korman NJ. Management of psoriasis as a systemic disease: what is the evidence? Br J Dermatol. 2020 Apr;182(4):840 -848.
- Svedbom A, et al. Skin Inflammation, Systemic Inflammation, and Cardiovascular Disease in Psoriasis. JAMA Dermatol. 2025;161(1):81 –86