Atopic dermatitis
Atopic dermatitis, or atopic eczema, is a chronic, non-contagious skin condition defined by inflammation and intense itching that typically worsens at night. The disease follows a recurrent pattern of flare-ups and remissions, presenting as dry, cracked, or brownish patches.
Its appearance shifts with age; infants usually develop small bumps on their cheeks, whereas older children and adults typically experience rashes on the scalp, hands, or within the folds of the elbows and knees. Because the condition compromises the skin barrier, patients face an increased risk of secondary bacterial and viral infections, often marked by crusting or the presence of pus.
While atopic dermatitis affects a significant number of children and adults globally, the majority of patients first exhibit symptoms during their first year of life. Although the number of new diagnoses continues to rise, a large portion of those who develop the condition in early childhood experience spontaneous remission before they reach adolescence. For those whose symptoms persist into adulthood, the disease requires ongoing management to control inflammation and prevent localized infections.



Types of atopic dermatitis
Clinicians categorized atopic dermatitis into two primary types based on the body's immune response: extrinsic and intrinsic. The extrinsic (allergic) type involves high levels of IgE (an antibody the immune system produces when it overreacts to allergens) and clear sensitization to external triggers. In contrast, the intrinsic (non-allergic) type presents with normal IgE levels and shows no specific allergic sensitivities.
Because no single laboratory test can determine the severity of the disease, doctors use a combination of objective and subjective tools to guide treatment. They rely on clinical scales like the EASI, SCORAD, and IGA to assess the extent of skin damage, while also evaluating patient-reported factors such as itch intensity and sleep disruption. These measurements allow healthcare providers to track how well a patient responds to therapy and adjust their care accordingly.

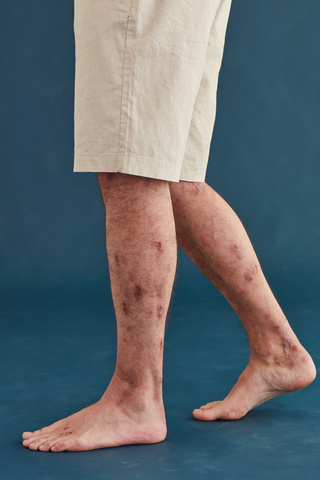
Vicente, living with Atopic Dermatitis
What causes atopic dermatitis?
The exact cause of atopic dermatitis is not completely clear. It may involve genetic and environmental factors leading to abnormalities in the epidermis and the immune system.
Atopic dermatitis can appear, or flare up, when a person is exposed to something in his or her environment. This is commonly called a trigger. Known triggers for atopic dermatitis include exposure to allergens, such as pollen, or stress, dry skin and infection. Skin irritants such as some fabrics, soaps and household cleaners may also trigger an atopic dermatitis flare-up.

Alicia, living with Atopic Dermatitis
How is atopic dermatitis diagnosed?
Doctors primarily diagnose atopic dermatitis through a physical examination and a detailed review of your medical history, as no specific blood test or scan can confirm the condition. They look for "essential" features, such as intense itching and the characteristic appearance of red, dry, or leathery patches in age-specific areas like the face in babies or the creases of the elbows and knees in adults. Your physician will also check for a "personal or family history of atopy", meaning they will ask if you or your close relatives suffer from asthma, hay fever, or food allergies. While clinicians occasionally use skin swabs to rule out bacterial infections or patch tests to identify contact allergies, they generally rely on established clinical frameworks, such as the UK Working Party criteria, to make a definitive diagnosis.
How to detect atopic dermatitis
Atopic dermatitis is defined by intense pruritus (itching) and skin inflammation that typically worsens at night, often leading to severe scratching and bleeding. As a primary diagnostic feature, this itching accompanies symptoms like dry, cracked, or eczematous patches. The disease’s appearance varies by age: infants typically develop bumps on the cheeks, while older children and adults experience rashes in joint folds, on hands, or on the scalp. Consequently, the relentless itching causes significant sleep disturbances, including insomnia and frequent waking. These sleep deficits often result in daytime drowsiness, irritability, and impaired concentration, potentially affecting growth and behaviour.
References
- Leung DY, Guttman-Yassky E. Deciphering the Complexities of Atopic Dermatitis: Shifting Paradigms in Treatment Approaches. J Aller Clin Immunol. 2014;134(4):769-79.
- Moyle M, Cevikbas F, Harden JL, Guttman-Yassky E. Understanding the immune landscape in atopic dermatitis: the era of biologics and emerging therapeutic approaches. Exp Dermatol. 2019;28(7):756-68.
- Eichenfield, L.F., Tom, W.L., Berger, T.G., Krol, A., Paller, A.S., Schwarzenberger, K., et al. Guidelines of care for the management of atopic dermatitis: section 2. Management and treatment of atopic dermatitis with topical therapies. J Am Acad Dermatol. 2014;71(1):116–32.
- Thomsen, S.F. Atopic Dermatitis: Natural History, Diagnosis, and Treatment. ISRN Allergy. 2014;2014:1–7.
- Avena-Woods C. Overview of atopic dermatitis. AJMC. 2017;1–10.
- Kowalska-Olędzka, E., Czarnecka, M., Baran, A. Epidemiology of atopic dermatitis in Europe. J Drug Assess. 2019;8(1):126–8.
- Nutten, S. Atopic dermatitis: global epidemiology and risk factors. Ann Nutr Metab. 2015;66:8–16.
- Williams, H.C. Clinical practice. Atopic dermatitis. N Engl J Med. 2005;352:2314–24.
- Sidbury, R., Davis, D.M., Cohen, D.E., Cordoro, K.M., Berger, T.G., Bergman, J.N., et al. Guidelines of care for the management of atopic dermatitis: Part 3: Management and Treatment with Phototherapy and Systemic Agents. J Am Acad Dermatol. 2014;71(1):116–32.
- Tokura, Y. Extrinsic and intrinsic types of atopic dermatitis. J Dermatol Sci. 2010;58(1):1-7. doi: 10.1016/j.jdermsci.2010.02.008.
- National Eczema Association (NEA). Atopic Dermatitis 101 [Internet]. 2016. Available at: https://nationaleczema.org/atopic-dermatitis-101/
- American Academy of Dermatology (AAD). Atopic dermatitis: symptoms [Internet]. 2020. Available at: https://www.aad.org/public/diseases/eczema/types/atopic-dermatitis/symptoms
- Gooderham, M.J., Bissonnette, R., Grewal, P., Lansang, P., Papp, K.A., Hong, C. Approach to the Assessment and Management of Adult Patients With Atopic Dermatitis: A Consensus Document. Section II: Tools for Assessing the Severity of Atopic Dermatitis. Journal of Cutaneous Medicine and Surgery. 2018;22(1S):10S-16S.
- Oszukowska, M., Michalak, I., Gutfreund, K., Bienias, W., Matych, M., Szewczyk, A., et al. Role of primary and secondary prevention in atopic dermatitis. Postep Derm Alergol. 2015;XXXII(6): 409–420. doi: 10.5114/pdia.2014.44017.
- European guideline: Wollenberg_2025_European Guideline (EuroGuiderm) on atopic eczema: living update