Palmoplantar pustulosis
Palmoplantar pustulosis, also called pustulosis palmaris et plantaris (PPP), is a rare non-contagious, chronic and inflammatory skin condition with an estimated prevalence of 0.050% to 0.12%. It is a localized form of pustular psoriasis, and is characterized by the appearance of painful sterile pustules (small skin lesions that contain pus) primarily in the palms of the hands and soles of the feet that erupt repeatedly over time. These pustules appear in conjunction with lesions that tend to crack, causing bleeding and pain.
In some cases, palmoplantar pustulosis also affects fingers and toes and causes nail lesions, and in severe cases some lesions may gradually enlarge and create patches that cover all the affected area. Affected individuals may also experience itching (pruritus), pain, or a burning sensation.
Signs and symptoms of palmoplantar pustulosis generally develop during adulthood (with the highest prevalence occurring between the ages of 50 and 69 years), and the condition is more common in women.



Types of palmoplantar pustulosis
Medical professionals do not typically divide palmoplantar pustulosis into distinct "types"; instead, they classify it by its clinical presentation and relationship to other diseases. Most patients experience the chronic-recurrent form, where yellow pustules appear in cycles, turn brown, and peel away over many years. Some specialists differentiate cases based on whether the condition occurs in isolation or as part of pustular psoriasis, where similar lesions appear elsewhere on the body. A specific, severe variant known as acrodermatitis continua of Hallopeau starts at the fingertips or toes and can eventually destroy the nails and underlying bone. While these variations exist, doctors primarily focus on the severity of the skin thickening and the frequency of the inflammatory flares to guide treatment.
What causes palmoplantar pustulosis?
The cause of palmoplantar pustulosis is currently unknown, but it is hypothesized to be a disorder of the eccrine sweat glands, which are most numerous on palms and soles, and that a combination of genetics (specifically, a mutation in the gene IL36RN appearing in around 5% of PPP patients), autoinflammatory, and environmental factors likely play a role in its development. In this regard, this disease is strongly associated with smoking: the majority of patients smoke or have smoked in the past (with an estimated (65–90%). It is thought that activated nicotine receptors in the sweat glands cause an inflammatory process.

How is palmoplantar pustulosis detected?
The appearance of pustules in the palms of the hands and soles of the feet is usually the most prevalent symptom of palmoplantar pustulosis. Diagnosis is usually easily made by healthcare professionals through visual examination. A skin biopsy (a procedure in which skin cells are removed for their examination) might be useful to rule out other health conditions.
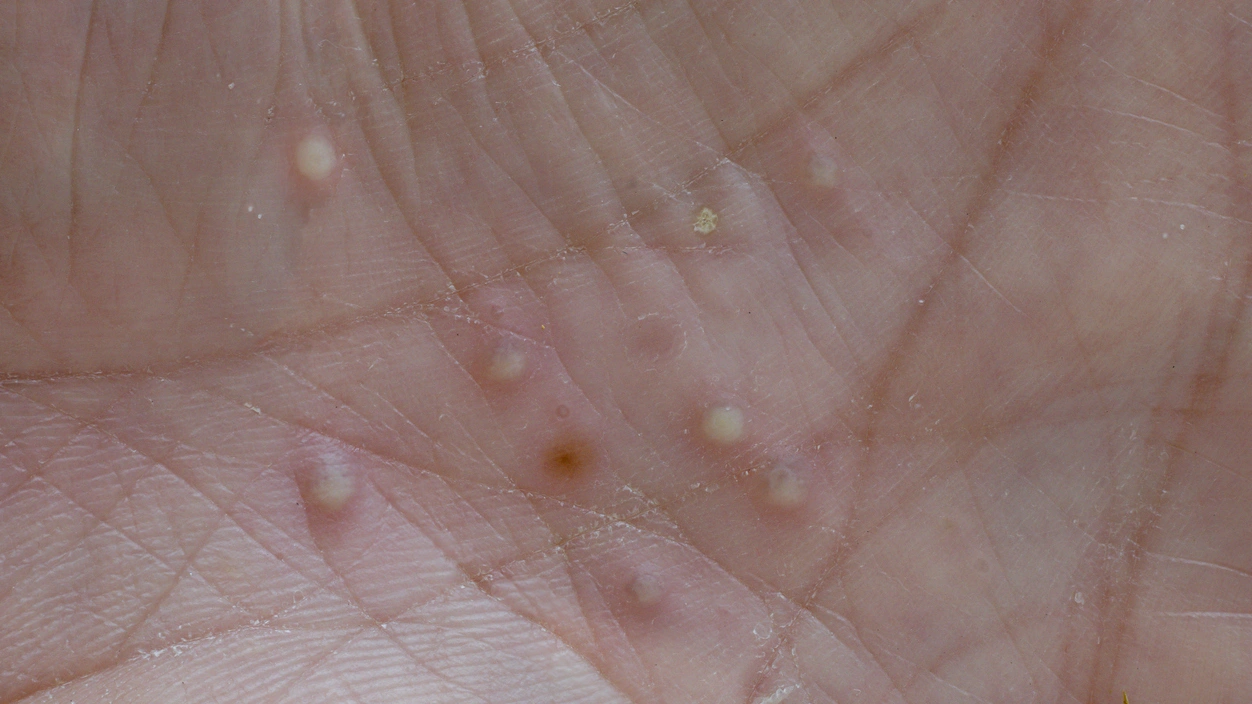
What does palmoplantar pustulosis look like?
Palmoplantar pustulosis appears as clusters of small, yellow-white pustules on reddened skin of the palms or soles. These blisters represent a localized inflammatory response where white blood cells accumulate under the skin. As the condition progresses, the pustules dry out and turn into dark brown, scaly crusts. This cycle leads to significant hyperkeratosis. Because the affected skin loses its elasticity, even simple movements like walking or gripping objects can cause intense discomfort or a burning sensation.

How is palmoplantar pustulosis treated?
Palmoplantar pustulosis lacks a specific cure or universally approved treatment in the US and EU, making clinical management particularly challenging. Current strategies focus on symptom alleviation through a combination of topical and systemic interventions. Topical corticosteroids are frequently employed for their anti-inflammatory properties, though their use is limited by potential side effects and decreasing efficacy over time. Other common options include phototherapy and oral retinoids for severe cases, alongside coal tar ointments to help prevent the reappearance of pustules. Additionally, the regular application of moistrurizing creams and ointments is essential to maintain skin elasticity and prevent the development of painful fissures.
References
- DermNet. Palmoplantar pustulosis. Available at: Palmoplantar pustulosis (localised pustular psoriasis) | DermNet (dermnetnz.org)
- Orphanet. Pustulosis palmaris et plantaris. Available at: Orphanet: Pustulosis palmaris et plantaris
- Genetic and Rare Diseases Information Center. Pustulosis palmaris et plantaris. Available at: Pustulosis palmaris et plantaris - About the Disease - Genetic and Rare Diseases Information Center (nih.gov)
- Brunasso AMG and Massone C. Recent advances in palmoplantar pustulosis. Faculty Reviews. 2021;10:(62). doi: 10.12703/r/10-62
- Kromer C. et al. Drug survival and reasons for drug discontinuation in palmoplantar pustulosis: a retrospective multicenter study. J Dtsch Dermatol Ges. 2019 May;17(5):503-516. doi: 10.1111/ddg.13834. Epub 2019 Apr 17. PMID: 30994260; PMCID: PMC6850581.
- Genovese G. et al. Pustular Psoriasis: From Pathophysiology to Treatment. Biomedicines. 2021 Nov 23;9(12):1746. doi: 10.3390/biomedicines9121746. PMID: 34944562; PMCID: PMC8698272.
