Palmoplantar pustulosis diagnosis
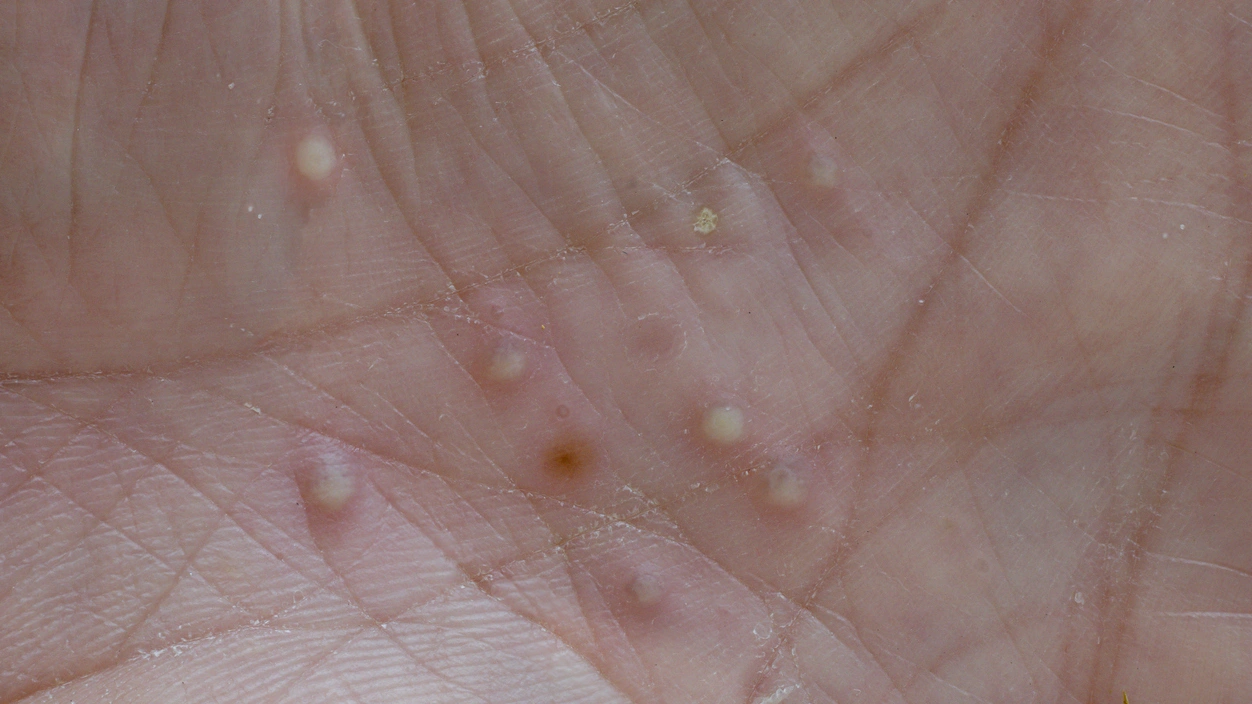
The accurate diagnosis of palmoplantar pustulosis (PPP) is essential to achieve effective treatment and to avoid unnecessary interventions. Its main characteristic is the appearance of recurrent sterile pustules, primarily on the palms of the hands and soles of the feet. Although it shares similarities with other pustular or eczema-related conditions such as psoriasis, clinicians rely on distinctive clinical features and targeted tests to diagnose palmoplantar pustulosis and differentiate it from other skin conditions.
How is palmoplantar pustulosis diagnosed?
Doctors typically begin the diagnosis of PPP with a clinical assessment. This involves taking a detailed history of symptoms and performing a thorough examination of the skin, particularly on the hands and feet. The doctor looks for the hallmark signs and symptoms of palmoplantar pustulosis, such as the sudden appearance of small, sterile pustules on reddened, scaly skin. These pustules are often surrounded by cracks or thickened skin. While the condition usually affects both palms or both soles symmetrically, it can appear asymmetrically in some cases.
In many instances, an experienced clinician can make a diagnosis based on these visible features, especially when the pattern of recurrent pustules, redness, and scaling is confined to the palms and soles. To avoid misdiagnosis, clinicians often ask about symptom patterns, potential triggers, family history of psoriasis or autoimmune conditions, smoking habits, and previous treatments.
Differentiating this disease from other similar conditions is crucial. Clinical judgement, supported by specific tests, when necessary, helps ensure an accurate diagnosis.
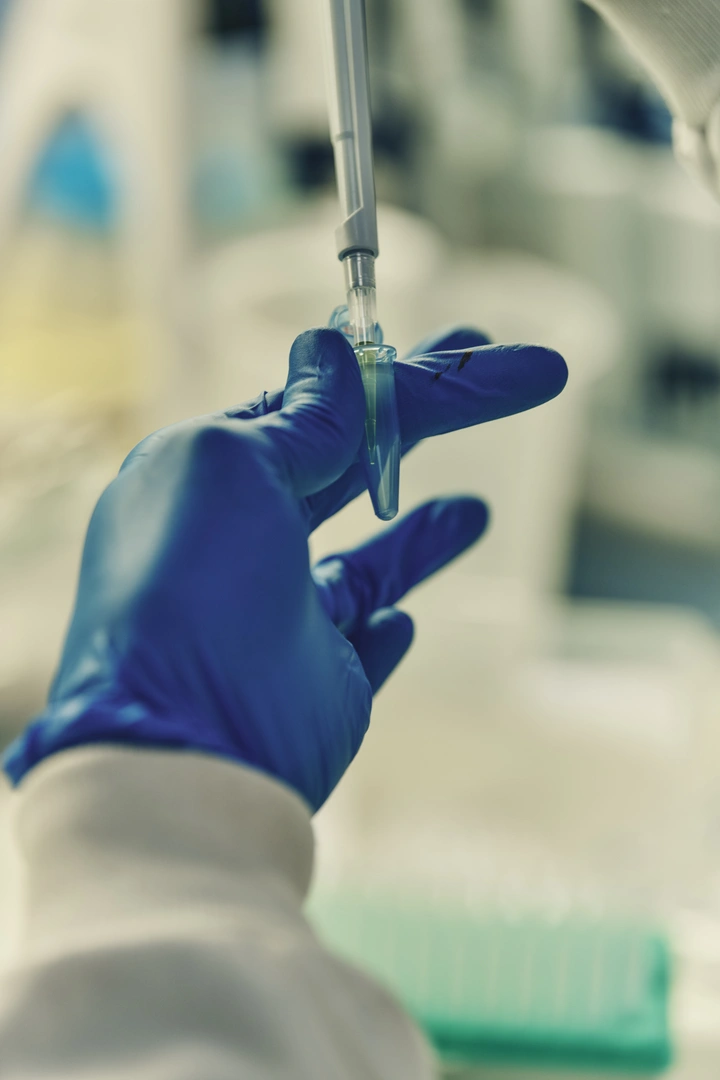
Skin scrapings and swabs
There are two main types of skin scraping and swabs that may be involved in the diagnosis of palmoplantar pustulosis:
Fungal test (Potassium Hydroxide Preparation)
A skin scraping is taken and treated with potassium hydroxide to detect fungal elements. This test helps rule out tinea (fungal infection), which can resemble PPP.
Bacterial and viral swabs
A swab taken from the fluid inside the pustules can be cultured to exclude bacterial or viral infections, confirming that the pustules are sterile and not caused by infection


Why clinical judgement matters
There is no single laboratory test that definitively diagnoses PPP. Instead, the diagnosis depends largely on clinical observation and the exclusion of other potential causes through targeted testing. Many individuals experience delays in diagnosis because PPP can be confused with conditions like eczema or other dermatoses, leading to inappropriate treatments before the correct diagnosis is made. Clinicians often monitor the condition over time, noting whether it responds to treatments that are typical for PPP management.
A precise diagnosis allows for more targeted treatment, including decisions about topical therapies, phototherapy, and systemic medicines. It also helps identify underlying factors, such as smoking, infections, or co-existing autoimmune conditions, that may influence disease activity and treatment choices.
References
- Freitas E, Rodrigues MA, Torres T. Diagnosis, Screening and Treatment of Patients with Palmoplantar Pustulosis: A review exploring clinical diagnosis and related recommendations. https://www.actasdermo.org/es-tratamiento-pustulosis-palmoplantar-con-ustekinumab-articulo-S1578219012000273 (Accessed 2025).
- Palmoplantar pustulosis: Epidemiology, clinical features and diagnosis — UpToDate: Overview of clinical features and diagnostic approach. https://www.uptodate.com/contents/palmoplantar-pustulosis-epidemiology-clinical-features-and-diagnosis (Accessed 2025).
- Freitas et al.: Clinical practices and recommendations in PPP including diagnostic methods — National Centre for Biotechnology Information. https://pmc.ncbi.nlm.nih.gov/articles/PMC7439281/ (Accessed 2025).