Hidradenitis suppurativa treatments
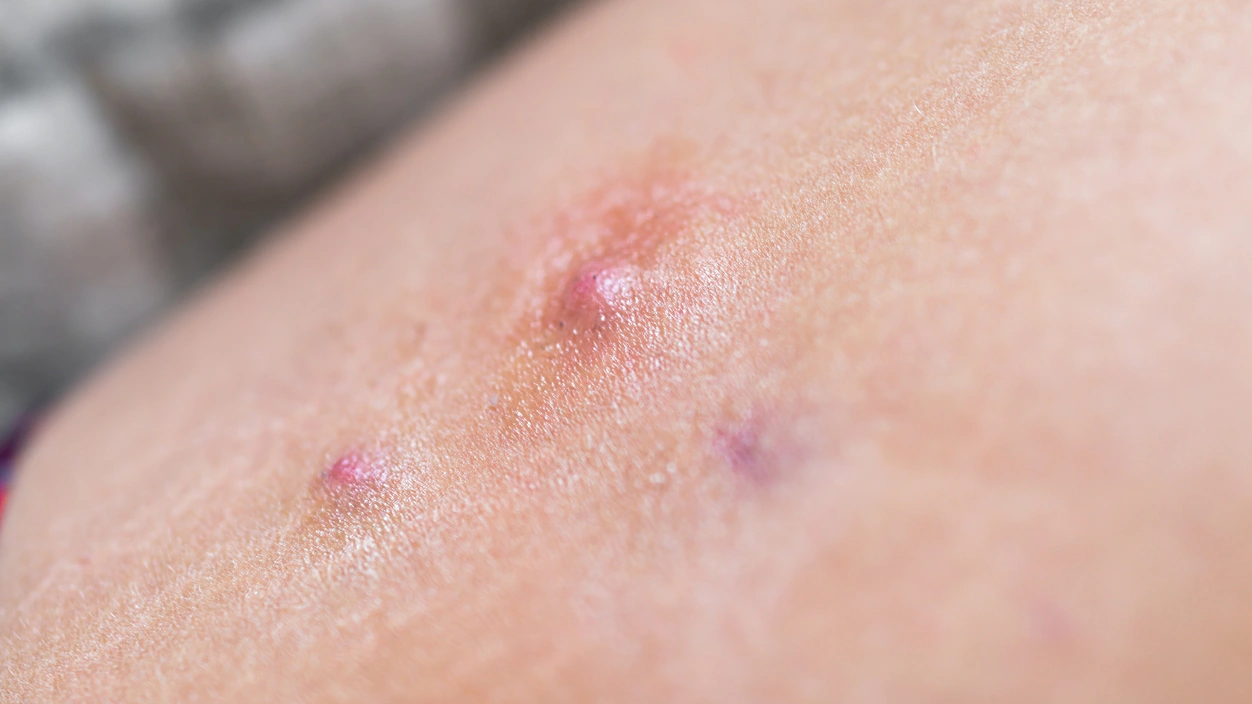
Hidradenitis suppurativa (HS) is a chronic inflammatory skin condition that produces painful nodules, abscesses, and tunnels under the skin. These usually appear in areas with many sweat glands, such as the armpits, groin, under the breasts, and around the buttocks. Because HS is usually chronic, painful, distressing to patients, and may lead to scarring,patients need consistent and effective treatment over time. Current guidance supports a combined approach that includes lifestyle adjustments, topical and systemic medicines and, when needed, procedures or surgery.
Does hidradenitis suppurativa have a cure?
There is currently no cure for HS. Most people live with a pattern of flare-ups and calmer periods. Early diagnosis of hidradenitis suppurativa and the use of targeted treatments can slow progression and reduce damage.
For many patients, the main goal is to control symptoms of HS, prevent new lesions, limit scarring, and improve quality of life. Some people do experience long periods with fewer symptoms, especially when they follow an individualized treatment plan and make supportive lifestyle changes.
What are the main treatments for hidradenitis suppurativa?
Clinicians tailor HS treatment to the severity of symptoms, the location of lesions, existing health conditions, and lifestyle factors. The main treatment categories include the following:
Antibiotics
Doctors often use oral and topical antibiotics in early and moderate HS because they reduce inflammation. Tetracyclines, such as doxycycline, and combinations like clindamycin with rifampicin, can reduce nodules and abscesses and may slow the condition’s progression. Topical clindamycin can also help when used regularly on smaller lesions.
In more severe or long-standing cases, clinicians may combine antibiotics with other systemic or biologic treatments.
Antiseptics
Antiseptic washes and topical antiseptics support broader treatment. Regular cleansing with products such as chlorhexidine or benzoyl peroxide can lower surface bacteria and may reduce the intensity of flare-ups. Antiseptics alone usually do not control moderate or severe HS, but they strengthen a wider routine, especially in milder disease.
Retinoids
Oral retinoids, particularly acitretin, can help some patients, although results vary. Clinicians usually consider them when other treatments fall short. Because retinoids can cause side effects, especially in women who may become pregnant, doctors monitor treatment closely. Retinoids may be most useful when HS occurs alongside acne-like skin changes.
Contraceptives
Hormonal treatments, including some contraceptive medications, can benefit patients whose HS worsens with hormonal fluctuations. Options that reduce reduce the impact of androgens may decrease the frequency and severity of flare-ups. This approach suits selected patients, particularly those who also experience symptoms such as acne or excess hair growth.
Immunomodulating treatments
Biologic and immune-modulating medicines now play a central role in moderate to severe HS. Adalimumab, a TNF-α inhibitor, has the strongest long-term evidence base and often reduces both lesion burden and pain. More recently, IL-17 pathway inhibitors have also been approved for HS, including secukinumab (IL-17A) and bimekizumab (IL-17A/IL-17F). Researchers continue to study newer biologic options and immune-targeted drugs.
Clinicians usually reserve these treatments for patients who do not respond to first-line therapies such as antibiotics, retinoids, or hormonal therapies.
Steroids
Steroids can offer short-term relief during acute flare-ups. Doctors may use topical steroids, steroid injections into active lesions, or occasional systemic steroids to calm inflammation and pain quickly. Long-term systemic use is discouraged because of their potential side effects and limited impact on the underlying condition. Steroids usually act as a temporary measure while longer-term treatments take effect.
Surgery
Surgery remains important for patients with more advanced HS marked by persistent tracts, scarring, and repeated abscesses. Options include deroofing, local excision, wide excision and, when required, grafts, or flap reconstruction. Surgery can provide long-lasting improvement when other treatments fail. Decisions about surgery usually involve both dermatologists and surgeons, and early referral can reduce long-term complications.
Laser and light therapy
Laser and light-based treatments offer additional options for patients who need more than medicines and surgery. Approaches such as Nd:YAG laser, CO₂ laser removal of tracts, and intense pulsed light (IPL) can lower inflammation and reduce recurrence. Some reviews show strong support for laser therapy as a non-surgical intervention. Although not a first-line choice for everyone, these therapies can make a significant difference when other methods fall short.
Overall, the choice of treatment for hidradenitis suppurativa depends on individual circumstances and often involves several approaches used together. Regular follow-up with a healthcare professional, realistic expectations about outcomes, and a focus on long-term management can help patients and clinicians work towards the best possible control of the condition.
References
- CUN. Hidrosadenitis supurativa. Available from: https://www.cun.es/en/diseases-treatments/diseases/hidrosadenitis-suppurativa
- Alikhan A, Sayed C, Alavi A et al. North American Clinical Management Guidelines for Hidradenitis Suppurativa: Part II: topical, intralesional and systemic medical management. J Am Acad Dermatol. (Accessible via PMC) PMC7105662. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC7105662/
- NHS. Hidradenitis suppurativa (HS). Available from: https://www.nhs.uk/conditions/hidradenitis-suppurativa/
- American Academy of Dermatology (AAD). Hidradenitis suppurativa treatment. Available from: https://www.aad.org/public/diseases/a-z/hidradenitis-suppurativa-treatment
- Frew JW, Navrazhina K, Piguet V. Therapies for hidradenitis suppurativa: a systematic review with a meta-analysis. PMC. 2022. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC8798365/