Alopecia areata diagnosis

Understanding the diagnosis of alopecia areata is important to ensure early identification, appropriate management, and clear differentiation from other forms of hair loss. Alopecia areata is a relatively common autoimmune condition characterized by sudden, patchy hair loss that does not damage the hair follicles. Although it does not cause physical pain, it can have a significant emotional and psychological impact.
How is alopecia areata diagnosed?
In most cases, the diagnosis of alopecia areata is made through a clinical assessment. This means that a healthcare professional, usually a dermatologist, identifies the condition based on visible signs and symptoms of alopecia areata and the patient’s medical history, rather than relying on laboratory tests alone.
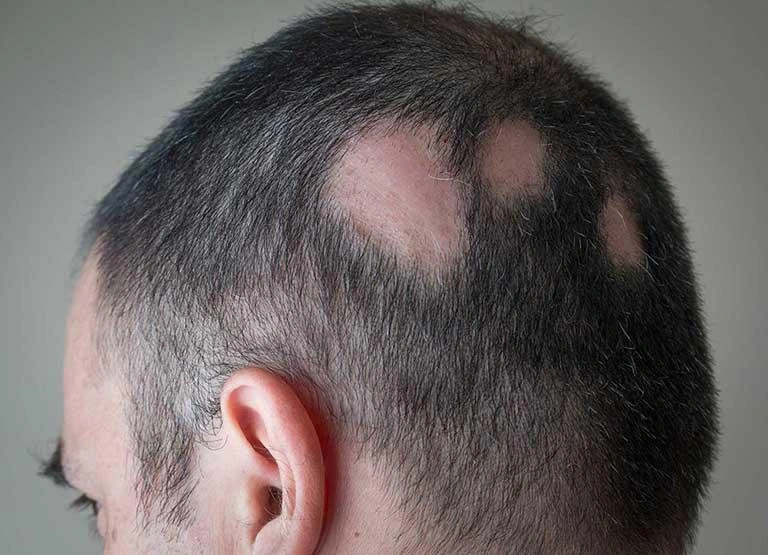
The most typical sign is the sudden appearance of one or more clearly defined round or oval patches of hair loss. These areas are usually smooth, with normal-looking skin underneath, and most commonly appear on the scalp. However, hair loss can also affect the eyebrows, eyelashes, beard, or other parts of the body. The absence of scarring or skin damage is a key feature and helps distinguish alopecia areata from other hair loss disorders that permanently damage hair follicles.
Specialist examination techniques, such as dermoscopy or trichoscopy, are often used to examine the scalp and hair more closely. These methods allow the clinician to see characteristic changes in the hair and follicles, including short broken hairs that narrow at the base, small dark points where hairs have broken off, and follicular openings filled with keratin. These findings strongly support a diagnosis of alopecia areata.

Taking a detailed medical history is also essential. Patients are typically asked when the hair loss began, how quickly it has progressed, whether there are any sensations such as itching or tingling, and whether they have experienced similar episodes in the past.
A family history of alopecia areata or other autoimmune conditions may also be relevant. In addition, a hair pull test may be performed. This involves gently pulling a small group of hairs to see how many are released, which can indicate whether the condition is currently active.
If the clinical signs are not clear, it may be necessary to resort to other tests.
Physical and dermoscopic or trichoscopic examination
A careful inspection of the scalp and hair is always the first step. Magnified examination techniques help identify patterns and structural changes in the hair and follicles that are typical of alopecia areata and not usually seen in other types of hair loss.
Hair pull test
This quick and simple test helps assess ongoing hair shedding. If a higher-than-expected number of hairs are easily removed, it suggests that the disease is active and progressing.
Scalp biopsy
A scalp biopsy is rarely needed but may be considered if the diagnosis is unclear or if the clinician suspects a scarring form of hair loss or other types of alopecia areata. A small sample of scalp tissue is examined under a microscope to look for inflammatory changes around the hair follicles that are consistent with alopecia areata.
Laboratory tests
Blood tests are not used to directly diagnose alopecia areata, but they may be helpful in identifying related conditions or alternative causes of hair loss. These tests may include assessments of thyroid function or markers of autoimmune activity, depending on the individual’s symptoms and medical history.
Screening for infections
If a clinician suspects a fungal infection of the scalp or another infectious cause of hair loss, they may perform additional tests such as fungal cultures or microscopic examination.
These tests help confirm the diagnosis of alopecia areata and rule out conditions that can appear similar, such as pattern hair loss, stress-related shedding, compulsive hair pulling, or scarring alopecias.
Rapid or patchy hair loss
Especially when smooth, round, or oval bald areas develop over a short period.
Unclear cause of hair loss
Particularly when the pattern does not match common types of thinning.
Additional symptoms
For example, itching, burning sensations, changes in the nails, or loss of eyebrows or eyelashes.
Emotional or psychological distress
Including anxiety, low mood, or reduced self-confidence related to hair loss.
Possible signs of underlying health conditions
For example, symptoms suggestive of autoimmune or hormonal disorders.
Seeking medical advice early allows for an accurate diagnosis and a discussion of treatment options for alopecia aerata. These may range from monitoring in mild cases to medical treatments aimed at reducing inflammation or stimulating hair regrowth in more extensive or persistent forms of the condition.
References
- Cleveland Clinic. Alopecia areata: symptoms, causes, treatment & regrowth [Internet]. Cleveland Clinic; last reviewed 2023 Aug 30 [cited 2025 Dec 12]. Available from: https://my.clevelandclinic.org/health/diseases/12423-alopecia-areata#diagnosis-and-tests
- Ma T, Zhang T, Miao F, Liu J, Zhu Q, Chen Z, et al. Alopecia Areata: Pathogenesis, Diagnosis, and Therapies. MedComm (2020). 2025 Apr 21;6(5):e70182. doi:10.1002/mco2.70182. Available from: https://onlinelibrary.wiley.com/doi/full/10.1002/mco2.70182
- Moussa A, Bokhari L, Sinclair RD. Alopecia areata: a review of diagnosis, pathogenesis and the therapeutic landscape. Wound Pract Res. 2022;30(1):24-33. doi:10.33235/wpr.30.1.24-33. Available from: https://journals.cambridgemedia.com.au/wpr/volume-30-number-1/alopecia-areata-review-diagnosis-path…;