Hidradenitis suppurativa types
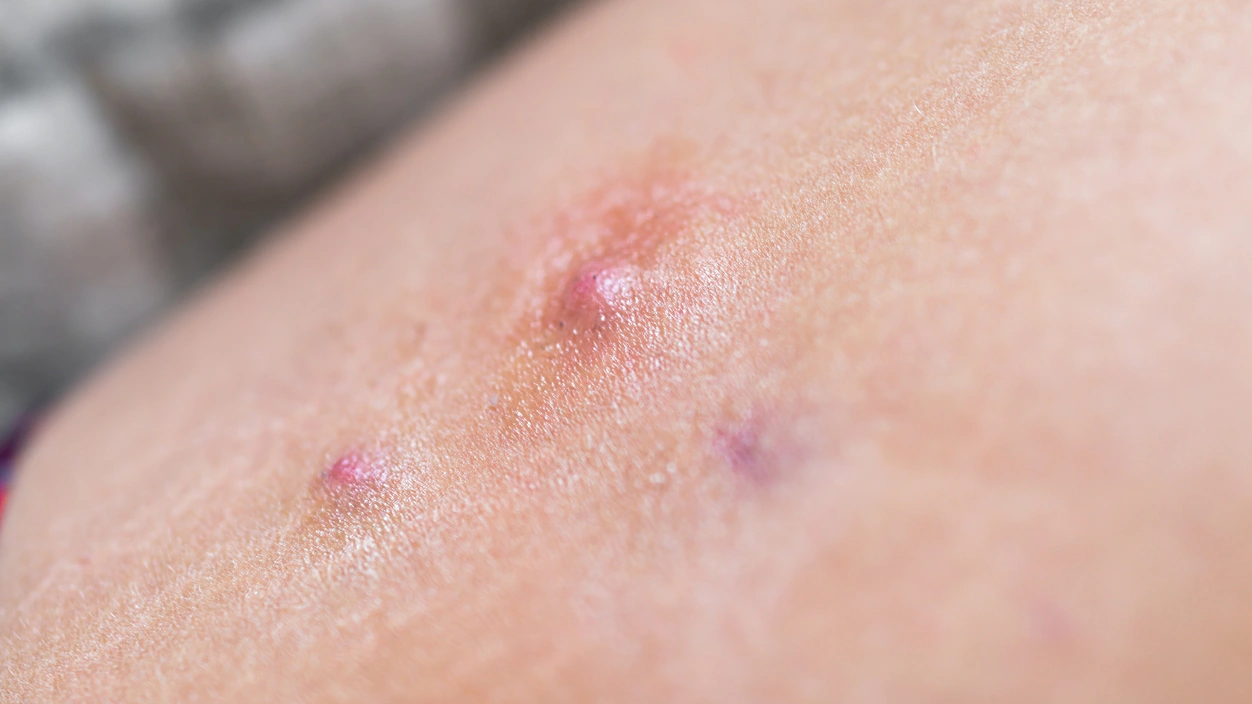
Hidradenitis suppurativa (HS) does not look the same in every person. Recognizing the different types of hidradenitis suppurativa helps clinicians assess how the disease may progress and choose the most appropriate treatment options, which is important because HS often has a substantial impact on daily life, affecting mobility, sleep, and psychological wellbeing.
What are the different types of hidradenitis suppurativa?
HS does not follow a single, uniform pattern. Instead, it presents as a spectrum of clinical forms that vary in severity, distribution of lesions, and associated conditions. There is no single classification system used in all settings, but specialists describe HS using several complementary approaches. These include phenotypic patterns, anatomical distribution, and research-based subgroups linked to comorbidities and inflammatory profiles.
Phenotypic classifications of HS
One of the most established ways to describe hidradenitis suppurativa focuses on two broad phenotypes: follicular and inflammatory. These terms describe how the disease behaves rather than acting as strict diagnostic labels.
- Follicular subtype: This form often appears earlier in life and mainly involves nodules. People with this presentation may also have acne or other follicular disorders. Abscesses tend to occur less frequently, and the disease course may progress more slowly.
- Inflammatory subtype: This presentation usually follows a more aggressive course. Patients experience recurrent, painful abscesses that may join up and form sinus tracts. Ongoing inflammation often leads to scarring, persistent discharge, and a higher level of physical discomfort and psychological distress.
Clinicians use these phenotypes to better understand disease behaviour and to guide decisions around the monitoring and the treatment of hidradenitis suppurativa.
Anatomical and clinical subtypes of hidradenitis suppurativa
Another approach classifies hidradenitis suppurativa according to where lesions develop and how they cluster across the body. A commonly cited framework describes four main clinical patterns:
- Axillary–mammary–inguinal subtype: Lesions mainly affect the armpits, under the breasts, and the groin. This pattern is more frequently seen in women, and hormonal factors may influence symptom severity and flare-ups.
- Follicular subtype: In this anatomical classification, HS appears alongside other follicular conditions and tends to involve widespread nodules.
- Gluteal subtype: This form primarily affects the buttocks and perianal region. The location can complicate management due to friction, moisture, and challenges with local care.
- Syndromic subtype: In a smaller group of patients, HS occurs as part of a broader autoinflammatory syndrome, such as PASH or PAPASH. These patients may also develop conditions like pyoderma gangrenosum or inflammatory arthritis, and often benefit from coordinated, multidisciplinary care.
These patterns help clinicians recognize less typical forms of HS and adapt treatment strategies to specific anatomical challenges.
Research-based subtypes
More recent studies have applied statistical and cluster analysis techniques to large patient groups to identify distinct HS subtypes. This research has described up to six clinical subgroups defined by shared comorbidities, inflammatory markers, and patient-reported outcomes. Examples include subtypes associated with diabetes, Crohn’s disease, asthma, psychiatric conditions, familial disease patterns, or a predominance in female patients.
Each subgroup shows differences in systemic inflammation, metabolic features, quality of life impact and response to treatment. These findings reinforce the idea that HS is not a single disease entity but a collection of related conditions with overlapping mechanisms. As research into genetic and molecular drivers continues, these classifications may support more personalized and targeted treatment approaches in the future.
How are the stages of hidradenitis suppurativa measured?
In addition to identifying clinical types, healthcare professionals assess HS severity using staging systems. These tools help guide treatment choices, monitor progression, and support communication between clinicians and patients. The most widely used system in routine practice is the Hurley staging system, valued for its clarity and ease of use.
Hurley staging
Hurley staging divides HS into three stages based on the extent of lesions, the presence of sinus tracts, and the degree of scarring.
Stage I
Patients develop single or multiple abscesses without sinus tracts or significant scarring. Lesions tend to remain isolated, and treatment often focuses on topical therapies and lifestyle measures.
Stage II
Recurrent abscesses occur alongside the formation of sinus tracts and scarring. Lesions may affect several separate areas. At this stage, the disease usually requires systemic treatment to control inflammation and reduce the frequency of flare-ups.
Stage III
The disease becomes widespread, with interconnected sinus tracts, multiple abscesses, and extensive scarring across affected areas. This advanced stage often requires surgical intervention alongside medical therapy.
Hurley staging allows clinicians to categorize HS as mild, moderate, or severe and to align treatment intensity with disease burden. It also provides a shared reference point for clinical research and patient discussions.

Other staging systems
Researchers have developed more detailed scoring systems to capture changes in HS severity over time. One example is the Sartorius score, which considers the number of lesions, the body areas involved, and the distance between lesions. These tools offer a more granular view of disease activity and can prove useful in clinical trials or when closely monitoring treatment response.
Emerging approaches also explore molecular and transcriptomic data to classify HS based on underlying biological differences. These methods may eventually refine how clinicians define HS subtypes and support truly personalized management strategies.
References
- Chadha M, Savage L. Hidradenitis suppurativa. DermNet [Internet]. 2025 Aug [cited 2025 Dec 15]. Available from: https://dermnetnz.org/topics/hidradenitis-suppurativa
- Petronelli M. Understanding hidradenitis suppurativa subtypes. Dermatology Times [Internet]. 2021 Sep 11 [cited 2025 Dec 15]. Available from: https://www.dermatologytimes.com/view/understanding-hidradenitis-suppurativa-subtypes
- AbbVie Inc. Hidradenitis suppurativa (HS) Hurley stages. HS Disease Source [Internet]. 2020 [cited 2025 Dec 15]. Available from: https://www.hsdiseasesource.com/hs-disease-staging
- Jørgensen AHR, Arildsen NS, Yao Y, Holm JG, Nielsen VW, Ring HC, et al. Cluster analysis identifies six clinical subtypes of hidradenitis suppurativa characterized by distinct comorbidities, inflammatory and metabolic profiles, patient-reported outcomes and treatment patterns. JEADV Clin Pract. 2023;2(1):80-91. doi:10.1002/jvc2.89 Available from: https://onlinelibrary.wiley.com/doi/full/10.1002/jvc2.89