Alopecia areata triggering factors
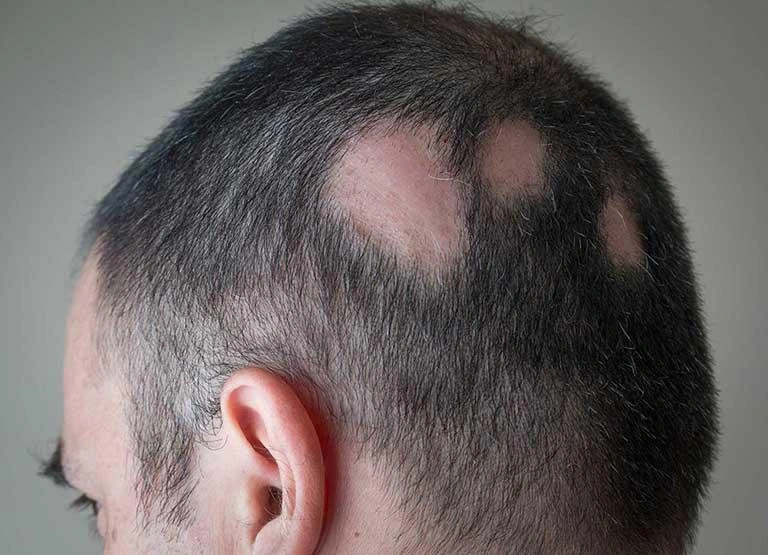
Who has a higher risk of developing alopecia areata?
Alopecia areata (AA) is an autoimmune condition in which the body’s own defence system mistakenly targets the hair follicle, disrupting its natural protection and leading to non-scarring hair loss. Although its precise origin is not yet fully understood, several well-established factors are known to increase an individual’s likelihood of developing the condition. Identifying these elements can support clinical assessment, patient education, and long-term monitoring.
A strong family history is one of the most consistent indicators of increased risk. People with close relatives affected by AA are more likely to develop the condition themselves. Research shows that AA is influenced by multiple genetic markers, and familial clustering often reflects a broader, polygenic susceptibility.
Individuals who already live with autoimmune or immune-related skin diseases face a higher risk of AA. Conditions such as psoriasis, vitiligo, and autoimmune thyroid disorders frequently occur alongside AA, suggesting overlapping immune mechanisms. Allergic and atopic tendencies are also more common in this group.
A history of atopic conditions such as eczema, asthma, or allergic rhinitis appears to increase vulnerability to AA. This association is believed to arise from shared patterns of immune imbalance, particularly involving pathways that regulate inflammatory responses.
Certain cancer treatments, especially those designed to alter immune activity, may trigger AA or speed up its onset in susceptible individuals. Therapies such as immune checkpoint inhibitors, or medicines that impact interleukin pathways, can occasionally disrupt hair-follicle immune regulation and contribute to hair loss.
Smoking
Current research links tobacco use with a noticeably higher incidence of AA. Longer-term smoking or heavier daily consumption appears to elevate risk even further. From a biological standpoint, smoking encourages inflammatory processes, disrupts immune balance, and may weaken the hair follicle’s natural protective environment.
Alcohol consumption:
The connection between alcohol and AA is less clear. Some findings indicate that alcohol may impact hormonal and immune responses in ways that, for certain individuals, could trigger or worsen symptoms. However, the evidence remains inconclusive and does not yet support specific clinical recommendations.
Sleep disturbance
Sleep problems — including poor sleep quality, chronic insomnia, or other sleep-related disorders — have been associated with a higher likelihood of AA, particularly among younger individuals. Insufficient or fragmented sleep can interfere with immune regulation, heighten systemic inflammation, and disrupt the hair-growth cycle.
Obesity
Excess body weight is increasingly recognized as a contributing factor. Obesity is often accompanied by low-grade, persistent inflammation and changes in metabolic signalling, both of which may play a role in weakening hair-follicle immunity and encouraging autoimmune activity.
Dietary fatty acids
The types and amounts of dietary fats consumed may influence AA risk. Diets rich in saturated fats and low in anti-inflammatory omega-3 fatty acids may tilt the immune system towards pro-inflammatory responses. Although the direct impact on alopecia areata is still being explored, this area highlights an emerging link between nutrition and immune-driven hair loss.
Gluten consumption:
Gluten intake has been examined due to its association with other autoimmune conditions, such as coeliac disease. While gluten does not appear to pose a problem for all individuals with AA, those who have confirmed gluten sensitivity or coeliac disease may benefit from dietary adjustments, as gluten can worsen immune-related inflammation in susceptible people.
Stress and other triggers
Emotional and psychological stress is one of the most commonly reported triggers of AA episodes. Stress hormones can disturb the hair follicle’s immune environment and promote inflammatory responses. Other triggers, including viral infections or broader immune challenges, may also contribute to episodes, although these sit outside lifestyle-related factors.
Alopecia areata arises from a complex interaction between genetic susceptibility, immune imbalance, and a range of potential triggers. While many risk factors cannot be changed, others – such as smoking, weight management, sleep quality, diet, and stress – may offer opportunities for intervention. Understanding these aspects can help patients and clinicians work together on more informed prevention strategies, realistic expectations, and supportive, holistic care.
References
- Minokawa Y, Sawada Y, Nakamura M. Lifestyle factors involved in the pathogenesis of alopecia areata. Int J Mol Sci [Internet]. 2022 [cited 2025 Nov 18];23(1038). Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC8835065/
- Sibbald C et al. Alopecia areata: An updated review for 2023. PMCID [Internet]. 2023 [cited 2025 Nov 18]. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10291119/
- Lintzeri D A et al. Alopecia areata – current understanding and management. Dermatology [Internet]. 2022 [cited 2025 Nov 18]. Available at: https://onlinelibrary.wiley.com/doi/10.1111/ddg.14689
- Akbaba E et al. Alopecia areata: a comprehensive review of clinical, aetiologic and therapeutic aspects. Dermatol Therapy [Internet]. 2025 [cited 2025 Nov 18];(2025-00013-8). Available at:https://link.springer.com/article/10.1007/s44368-025-00013-8